
Want to ease pressure in urgent care? Simply cut community services!?!
What should decision makers do with analysis that challenges deeply held assumptions? In this blog, Fraser Battye reflects on a surprising recent finding about community services.

Ghosted by an old friend
“…personal contact was a vital element in general practice from the beginning. By 1959 50% of people in England regarded their GP as a personal friend.”

Part-time GPs and the decline in continuity of care: a cause or a symptom?
In our recent paper we explore why levels of care continuity have been declining and what might be done to turn things around.

Two sides of the same coin
Hospital demand arising from GPs not seeing patients, is eating into the resources that they would use to manage down the elective backlog. In turn, this is creating more demand for GPs.

Are GP consultation rates rising or falling? Who or what should we believe?
If the "data suggests" GP appointments are substantially higher than pre-pandemic, then what is behind patients reporting recieving fewer appointments?

GP services: new analysis and fresh insights
In our latest analysis for the Midlands Decision Support Network (MDSN), we explore the long standing problem of access to GP practice consultations we consider the implications, and explore potential solutions.
Socio-economic inequalities in coronary heart disease
There are substantial differences in mortality rates from cardiovascular disease between socio-economic groups. Our new tool provides an overview, for ICBs, of the points on the care pathway where inequalities emerge and are amplified

The impact of social care on demand for urgent hospital care: have we reached a consensus?
The care home COVID crisis and the effects of longstanding staffing and funding shortages has meant that social care has featured heavily in the media over the last 12 months.
Some positive news for integrating GP practices with hospital trusts
The drive for greater integration of health and care services has been the central theme of UK health policy for most of
Lessons, Evaluation and Learning from the Dudley MCP
Learning from Dudley MCP
Lessons from the Vanguard: Innovation and Evaluation
The problems facing health and care services are so well known as to be documented in the media most days.
Lessons from the Vanguard: Procurement
Evaluation of the Dudley New Care Models Programme
This is the final system-wide report from the evaluation.
Horizontal or Vertical: Which way to integrate?
In 2011, Primary Care Trusts faced a difficult choice. The Transforming Community Services policy required a complete break of commissioner and provider functions. But what should PCTs do with the community health services they delivered; vertically integrate with an acute trust, horizontally integrate with a mental health trust, or set up a stand-alone community trust or Community Interest Company? Seven years on, this report explores the impact this choice had on the level and growth in emergency hospital use in older people and considers the wider implications for the NHS as it develops new models of care and integrated care systems

Scenario planning – an antidote to the false certainties of forecasts and grand plans
The resurgence of uncertainty

Scenario planning – an antidote to the false certainties of forecasts and grand plans
The resurgence of uncertainty
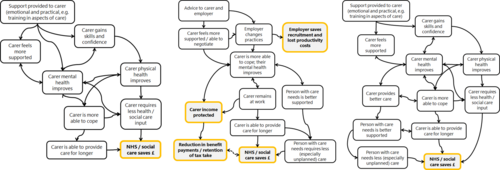
Scoping study: the economics of caring
There is a clear moral case for supporting unpaid carers.
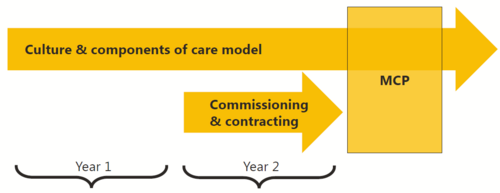
Dudley MCP Evaluation of New Schemes
To support the move to the MCP model of care, Dudley's Partnership Board instituted a series of new schemes.
Evaluation of the Dudley Multidisciplinary Teams (MDTs) Summary of Final Report
Multi-disciplinary Teams (MDTs) in primary care are a core component of Dudley's care model; they are also widely used elsewhere.
