
Part-time GPs and the decline in continuity of care: a cause or a symptom?
In our recent paper we explore why levels of care continuity have been declining and what might be done to turn things around.

Two sides of the same coin
Hospital demand arising from GPs not seeing patients, is eating into the resources that they would use to manage down the elective backlog. In turn, this is creating more demand for GPs.

Are GP consultation rates rising or falling? Who or what should we believe?
If the "data suggests" GP appointments are substantially higher than pre-pandemic, then what is behind patients reporting recieving fewer appointments?

GP services: new analysis and fresh insights
In our latest analysis for the Midlands Decision Support Network (MDSN), we explore the long standing problem of access to GP practice consultations we consider the implications, and explore potential solutions.

A Picture of End-of-Life Care in England
Working with Macmillan our analysis investigates who is more likely to experience poor outcomes associated with shortcomings in end-of-life care? Are there particular areas in England where those at end-of-life face significant challenges and how might the supply of services in an area be influencing these?

A collaborative partnership with the Health Foundation
The Strategy Unit is collaborating with the Health Foundation to help address key health and social care issues by combining our expertise in data analysis.
How is growth in diagnostic testing affecting the hospital system?
Diagnostic services, such as medical imaging, endoscopy, and pathology, have grown substantially in recent years and at a faster rate than most other healthcare services. Increased diagnostic testing brings benefits to patients, but rapid growth of this service area within a complex, adaptive system such as the NHS is likely to have had unintended consequences. Midlands ICBs wanted to understand the impact of diagnostic growth on hospital services.
Socio-economic inequalities in coronary heart disease
There are substantial differences in mortality rates from cardiovascular disease between socio-economic groups. Our new tool provides an overview, for ICBs, of the points on the care pathway where inequalities emerge and are amplified

Infant-feeding problems during the pandemic
Emergency department attendances fell dramatically and systematically during the early phases of the COVID-19 pandemic. This effect was almost universal, affecting people from all parts of society and for all health conditions. But in our recent paper we highlight one notable exception to this rule -presentations at Emergency Departments for infant-feeding problems increased during the pandemic.
Inequalities in access to healthcare - what’s our next move?
Our research, published in the Lancet Regional Health Europe, highlights substantial inequities in access to elective hip replacement surgery. We found no evidence that these inequities reduced between 2006 and 2016.

Strategies to reduce inequalities in access to planned hospital procedures
UPDATE 10th August: Now including briefing note for Integrated Care Boards on legal duties in respect of reducing inequalities. This report guides ICBs through the process.

Advancing the analytical capability of the NHS and its ICS partners
The Strategy Unit were asked by the Strategy and Development Team in the Directorate of the Chief Data and Analytics Officer, NHSE/I, to make recommendations for advancing analytical capability across the health and care workforce.

Strategy Unit devises a new method for classifying outpatient appointments
The number of outpatient attendances in England is now approaching 100 million each year.

Infant feeding problems, lockdown and attendance at Emergency Departments: what’s going on?
From our previous work, with Nuffield Trust and Health Foundation, we know that lockdown had a significant effect on attendance at Emergency Departments (ED). We also know that this effect was very unevenly distributed: some demographic groups stayed away far more than others.

Decisions to admit patients are not solely determined by clinical risk
Whether or not to admit a patient is one of the most routine yet important decisions a doctor in an Emergency Department

Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
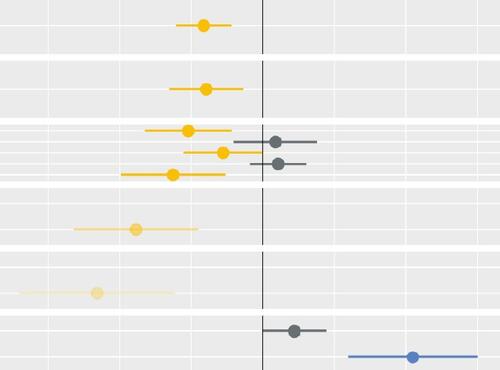
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.
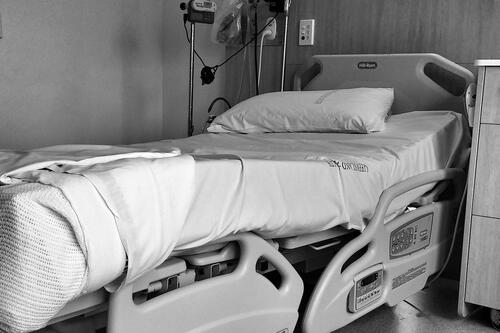
Strategy Unit analysis published showing changes in use of emergency departments under lockdown
We know that patterns of access to healthcare have changed during the pandemic.
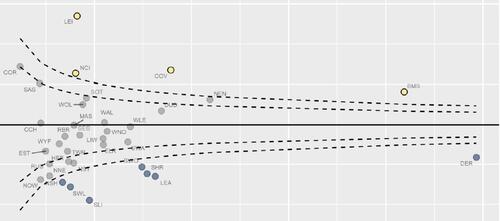
Equity and Cost Growth in Specialised Services
NHS specialised services provide care for people with complex or rare medical conditions.
